Most athletes should rest for 24–48 hours after a concussion, then begin light, symptom-guided exercise within the first week. Research shows that early, controlled movement actually speeds up recovery — the old “dark room for a week” approach is outdated. Athletes should follow a 6-step Return to Play protocol with a healthcare provider before returning to full competition. Sports physical therapists in Farmingdale, NY at In Motion Physical Therapy can guide athletes through a safe, evidence-based concussion recovery plan.
You took a hit. Your head is pounding. Someone tells you to go home, rest, and stay off your phone. And now you’re lying in a dark room wondering: how long do I actually have to wait before I can move again?
If you’re a competitive athlete, that question isn’t just about comfort. It’s about your season, your scholarship, your teammates counting on you. The fear of missing time — and the frustration of not knowing the real answer — is real.
Here’s the good news: the science has changed. What we now know about how long you should wait to exercise after a concussion is very different from what coaches and parents were told even five years ago. And the answer is probably better than you’re expecting.
→ Book a Discovery Call to get a baseline concussion assessment and a return-to-sport plan you can trust.
How Long Should You Wait to Exercise After a Concussion? What the Research Says
For years, the standard advice for concussion recovery was total rest — dark room, no screens, no activity — until every symptom disappeared completely. While the instinct to protect a healing brain makes sense, the research now tells us that prolonged inactivity can actually slow recovery down.
A landmark study published in JAMA Pediatrics by Leddy et al. (2019) found that teenagers who started light aerobic exercise — like walking or stationary biking — within the first week of a concussion recovered approximately four days faster than those who only did passive stretching. That’s a significant difference for an athlete staring down a two-week countdown to their next game.
The takeaway: movement, when done correctly and at the right time, is not dangerous after a concussion. It’s actually a form of treatment.
Step 1: The 24–48 Hour Rest Window
Before we talk about exercise, let’s be clear about one thing: the first 24 to 48 hours after a concussion are non-negotiable rest time.
Your brain just sustained an injury. During this short window, your neurons are in a state of metabolic crisis — they need energy to heal, and any extra demand (physical or cognitive) takes resources away from that process. This means:
- No practice, no gym, no running
- Reduced screen time (phones, tablets, TV)
- Avoiding cognitively demanding tasks like studying for exams
- Prioritizing sleep
This 24–48 hour rest period is supported by both the University of Michigan Health guidelines and the CDC HEADS UP concussion protocol. Think of it as giving your brain a genuine “timeout” before you start testing it again.
What this is not: a week in a dark room. Two days of rest is very different from two weeks of complete isolation — and the evidence does not support the latter.
Step 2: When to Start Exercising After a Concussion
After the initial rest window, the goal is to introduce light movement as soon as you can do so without making your symptoms worse. Research from Lempke et al. (2023) published in Sports Medicine showed that athletes who started light activity within the first few days recovered significantly faster than those who waited 8 or more days to move.
Waiting too long isn’t just frustrating — it’s counterproductive. Prolonged inactivity after a concussion has been associated with longer symptom duration and a higher risk of post-concussion syndrome, where symptoms drag on for a month or more.
The right approach is what clinicians call subthreshold exercise — movement that stays just below the level where your symptoms get worse.
What Is Subthreshold Exercise?
Think of your symptoms like a speedometer. Your job is to keep the needle below the red zone.
If you can walk at a comfortable pace and your headache stays the same or improves — that’s subthreshold. That movement is safe and helpful.
If jogging for two minutes makes your head throb or your vision go blurry — that’s above your threshold. Slow down, stop, and try again tomorrow at a lower intensity.
The CDC HEADS UP protocol (2025) recommends using a simple symptom rating scale (0–10) to track how you feel before, during, and after exercise. If your score increases by 2 or more points, that’s your signal to stop. Rest until symptoms settle, then return to the previous step of your plan.
This is not guesswork. It’s a measurable, repeatable process — and it’s exactly the kind of monitoring a sports physical therapist can help you navigate safely.
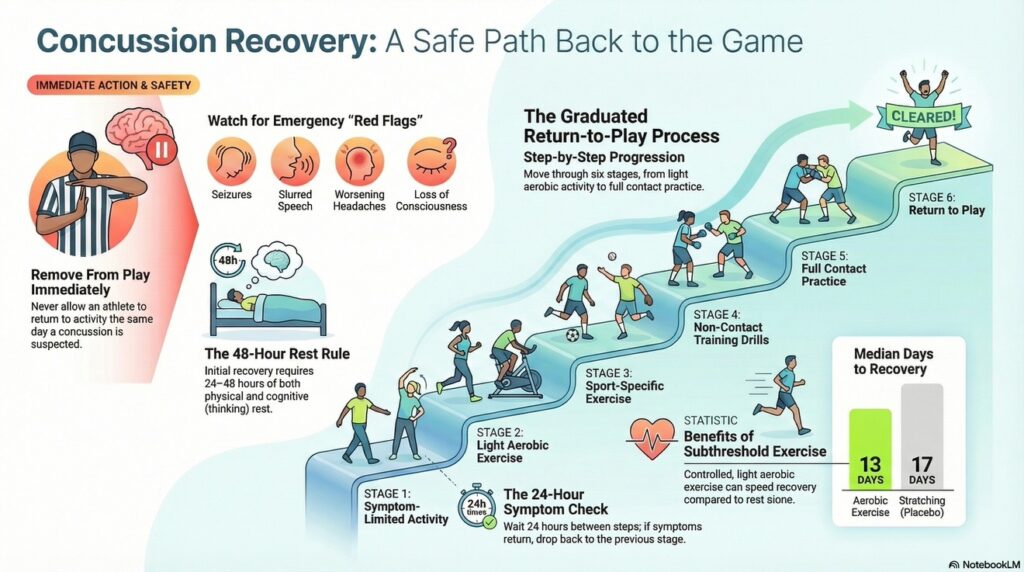
The 6-Step Return to Play Protocol
Returning to your sport after a concussion isn’t a light switch — it’s a ladder. The CDC HEADS UP guidelines outline a structured 6-step Return to Play (RTP) protocol, and the rule is simple: you need to spend at least 24 hours at each step without any symptoms before advancing to the next one. If symptoms return, you go back one step and wait again.
Here’s what that ladder looks like:
Step 1 — Symptom-Limited Activity Rest. Daily activities that don’t provoke symptoms. No physical exertion. (This is your 24–48 hour window.)
Step 2 — Light Aerobic Exercise Walking, swimming, or stationary biking at low intensity. No resistance training yet. Goal: increase heart rate gently.
Step 3 — Sport-Specific Exercise Running drills, skating drills — movement patterns specific to your sport. Still no contact or heading/impact.
Step 4 — Non-Contact Training Drills More complex drills. Begin resistance training. Coordination and cognitive demands increase.
Step 5 — Full-Contact Practice After medical clearance. Normal training activity resumes.
Step 6 — Return to Competition Full game play.
Each step takes a minimum of 24 hours. Rush the ladder, and you risk going back to the bottom.
Red Flags: Stop Exercising Immediately If You Notice…
Exercising at a subthreshold level is safe — but there are warning signs that mean you need to stop and get evaluated right away. These are not symptoms to push through:
- Headache that suddenly worsens during exercise
- Dizziness or loss of balance
- Visual disturbances (blurry vision, double vision, seeing spots)
- Nausea or vomiting
- Feeling confused, foggy, or “not yourself”
- Neck pain that increases with activity
- Feeling significantly worse the next day
If any of these occur, stop the session immediately. Rest until all symptoms fully resolve, then drop back one step in your Return to Play progression. If symptoms are severe or don’t settle, seek medical evaluation.
“My Headache Stopped — Am I Cleared to Play?”
This is one of the most common and most dangerous assumptions athletes make: if my head doesn’t hurt, I’m fine.
A headache clearing is a good sign — but it’s not the finish line. A proper return-to-play clearance involves evaluating balance, reaction time, cognitive processing speed, and sport-specific physical demands. The University of Michigan Health guidelines (2026) are clear that a full clinical assessment — not just a pain check-in — is required before returning to contact sport.
At In Motion Physical Therapy, our concussion assessments include monitoring heart rate, symptom response to exertion, and cognitive function before and after exercise — not just asking “how’s your head feeling?” We’re exercise experts, and our job is to make sure that when you go back to your sport, your brain is genuinely ready — not just symptom-free for one afternoon.
How Sports Physical Therapy Helps Concussion Recovery
A sports PT plays a specific and important role in concussion recovery that goes beyond what a general practitioner can offer in a 15-minute office visit. Here’s what working with a PT means for your recovery:
Baseline and follow-up assessment. We monitor your symptoms, balance, blood pressure response to exercise, and cognitive function throughout the recovery process — not just at the start and finish.
Exercise prescription. We determine exactly what intensity of movement is safe for you on any given day, based on how your body is actually responding — not a one-size-fits-all protocol.
Cervicogenic symptom management. Many concussion symptoms — especially headaches and neck pain — have a cervical spine component that responds very well to manual therapy and targeted exercise. This is often missed in standard concussion protocols.
Return-to-sport confidence. One of the most underappreciated parts of concussion recovery is psychological. Athletes who go through a structured, supervised return-to-sport program report feeling far more confident and ready when they step back on the field.
Frequently Asked Questions about Exercising After a Concussion
How Long Should You Wait to Exercise After a Concussion?
Can exercise make a concussion worse?
What kind of exercise is safe after a concussion?
Does a concussion always require time off school or work?
When do I need medical clearance to return to contact sport?
How does a sports PT help with concussion recovery?
Next Steps: Don’t Guess Your Way Back
Returning to your sport after a concussion is not something you should navigate alone — or in a dark room, waiting for your headache to disappear.
The latest research is clear: with proper guidance, most athletes recover faster when they start moving early and follow a structured plan. The goal isn’t to keep you out of the game. It’s to get you back the right way — so you stay back.
At In Motion Physical Therapy in Farmingdale, NY, we work with competitive athletes at every stage of concussion recovery. From baseline assessment to full return-to-sport clearance, we build individualized plans that respect your timeline while making sure your brain is actually ready.
→ Book a Discovery Call to get a concussion assessment and a return-to-play plan built around your sport.
→ Learn more about our Sports Physical Therapy services
This post is for educational purposes only and does not constitute medical advice. If you or your athlete has sustained a concussion, seek evaluation from a qualified healthcare provider before returning to any physical activity.
Next on your Reading List:
References
- Leddy, J. J., et al. (2019). Early Targeted Heart Rate Aerobic Exercise Versus Placebo Stretching for Sport-Related Concussion in Adolescents. JAMA Pediatrics, 173(4), 319–325. https://pubmed.ncbi.nlm.nih.gov/30715132/
- Lempke, L. B., et al. (2023). Early Symptom Burden and Activity Following Sport-Related Concussion. Sports Medicine. https://pubmed.ncbi.nlm.nih.gov
- CDC HEADS UP Concussion Protocol (2025). https://www.cdc.gov/headsup
- University of Michigan Health — Concussion Recovery Guidelines (2026). https://www.uofmhealth.org

Laura Sommer has been practicing as a Physical Therapist since 2011. She graduated from Northeastern University, where she was a member of the Women’s Soccer Team. Laura is the owner of In Motion Physical Therapy located in Farmingdale, NY.




